Genetic screening tests are available to all pregnant women to assess whether they have an increased or decreased risk of having a baby with a genetic abnormality. There are options that include blood tests, ultrasounds and more invasive tests such as chorionic villus sampling and amniocentesis. All of these options are available to all pregnant women regardless of age, personal or family history or without a previous abnormal screening test result. These tests have been developed after many years of research and are updated constantly to allow them to detect more babies with genetic abnormalities. Some of the tests can have false positive results, meaning the test indicates that the pregnancy is at an increased risk for a genetic abnormality however further testing does not show an abnormality. It is helpful when choosing to have genetic screening to decide whether you are looking for reassurance that a screening test can give if it shows a significantly decreased risk of having a baby with a genetic abnormality. Or, if you are looking for a definite answer, such as given with chorionic villus sampling or amniocentesis.
Conditions that can be diagnosed prior to conception:
Genetic carrier testing allows prospective parents to evaluate their genetic carrier status for the four most common inherited disorders: cystic fibrosis (CF), spinal muscular atrophy (SMA), duchenne muscular dystrophy (DMD), and fragile X syndrome. These four conditions can cause serious health consequences, leading to decreased life span, impaired mental capability or even death. A specimen of your DNA is collected by either a blood or saliva sample.

Conditions that can be diagnosed by currently available genetic testing during pregnancy:
- Trisomy 21 is caused by an extra copy of chromosome 21 and is called Down syndrome. The condition is the most common cause of intellectual disability, and it may cause heart defects, other organ defects, and hearing or vision problems.
- Trisomy 18 is caused by an extra copy of chromosome 18 and is called Edwards syndrome. The condition causes severe intellectual disability along with serious defects of the heart, brain and other organs. Babies with Edwards syndrome usually survive less than one year.
- Trisomy 13 is caused by an extra copy of chromosome 13 and is called Patau syndrome. The condition causes severe intellectual disability and many serious birth defects. Babies with Patau syndrome usually survive less than one year.
- Monosomy X is caused by a missing X chromosome and is called Turner syndrome. The condition affects only females, and may cause heart defects, hearing problems, stunted growth, infertility, and minor learning disabilities.
Genetic Testing Available in the First Trimester:
The Fetal DNA Blood Test:
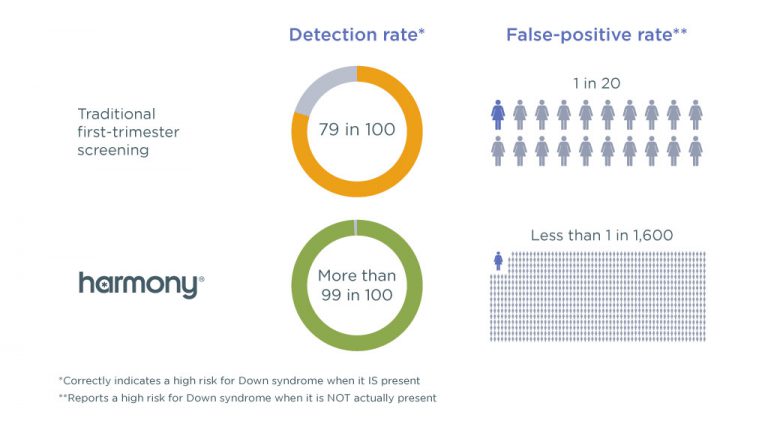
This is a prenatal blood test that can determine with a high degree of accuracy if your baby is at risk for Trisomy 21, 18,13, Triploidy and Monosomy X. Fetal DNA testing also evaluates the sex chromosomes, which can tell you the sex of the baby.
First Trimester Screening Test:
This test determines if your baby is at increased risk for Down Syndrome and Edwards Syndrome, as described above and is done between 10-13 weeks of pregnancy. The test includes an ultrasound to measure nuchal translucency, or the area of fluid at the back of the baby’s neck. Blood work is also drawn from the mother to measure two proteins, HCG and PAPP-A. These blood levels are combined with the ultrasound results to determine if the baby is at increased risk. This test has a false-positive rate of approximately 5% and does not give a definite diagnosis. Other anatomical abnormalities that are not genetic, can also be seen on this early ultrasound. If your test result indicates an increased risk for a chromosomal abnormality, you may decide to have further testing such as chorionic villus sampling or amniocentesis for a definite diagnosis.
Chorionic Villus Sampling:
Chorionic villus sampling (CVS) can be done if the first trimester test shows an increased risk for a genetic abnormality, in women over age 35 or women who have had a prior pregnancy or a family history of a genetic abnormality. CVS is generally done between 10-12 weeks of pregnancy. It is invasive testing and has a risk of miscarriage of 1 in 100. It involves obtaining a small sample of chorionic villi from the placenta to determine if the cells have the proper number and arrangement of chromosomes. Other risks include bleeding and a rare risk of infection. It may take 1-2 weeks to get results. CVS can have a false positive result in 1-2 % of the tests. Results may be confirmed by amniocentesis. If CVS indicates that your baby has a chromosomal abnormality, your health care provider or a genetic counselor can help you understand the results.
Genetic Testing Available in the Second Trimester:
Level II Ultrasound:
A level II ultrasound is an ultrasound that looks at the baby in closer detail for any anatomical changes that can be associated with certain genetic abnormalities. Heart, brain and other defects that have been associated with genetic abnormalities can often be seen with level II ultrasounds. These ultrasounds can be reassuring, however unfortunately with Down syndrome for instance; there can be as many as 50% of babies that do not have any obvious defects seen on ultrasound.
Amniocentesis:
An amniocentesis can diagnose Down syndrome, trisomy 18, spina bifida and other genetic abnormalities. It is generally done after 15 weeks of pregnancy. Amniocentesis is recommended if you have an abnormal first or second trimester screening test, in women over age 35, or women who have had a prior pregnancy with, or family history of, a genetic abnormality. It is invasive testing and has a risk of miscarriage of 1 in 300 to 1 in 500. It involves drawing a sample of amniotic fluid with ultrasound guidance to determine if the cells have the proper number and arrangement of chromosomes and to measure the amount of a protein called alpha-fetoprotein. Other risks include bleeding, infection, amniotic fluid leakage and needle injury to the baby. An amniocentesis cannot identify all birth defects as some birth defects are not associated with a chromosomal abnormality. If your amniocentesis results indicate that your baby has a chromosomal abnormality or spina bifida, your health care provider or a genetic counselor can help you understand the results.